Vegan Sources of Calcium
Past president of the American College of Lifestyle Medicine (ACLM), Dr. George Guthrie, MD, explains the different vegan sources of calcium and how best to obtain it.

What is calcium?
Calcium is one of the most abundant elements on the planet, with entire islands being made from calcium carbonate. Shells, coral, and our bones get their structure from calcium carbonate.
When vitamin D is present, our bodies absorb dietary calcium fairly well. Calcium levels in the blood must be kept in near-perfect range or serious health problems can occur.
Nerves and muscles can get irritable when the levels vary, which can lead to deadly heart arrhythmias, muscle spasms, seizures, or worse. Our body has at least two systems that work together to keep that level steady. For that reason, a blood test cannot determine whether we are getting enough calcium in our diet.
Best vegan sources of calcium
What whole, plant-based foods contain calcium?
The dairy industry claims that calcium comes from milk and that it is vitally important to get enough. In a whole-food, plant-based diet, milk is avoided (or minimized) because of the problems caused by animal proteins.
So, where will we get calcium if we’re not consuming milk? Each glass of milk contains around 400 mg of calcium. The RDA for teenagers is 1,300 mg and, for people age sixty-five and older, 1,000 mg. Three glasses of milk should supply that. Or this is what we’ve been told. But wait a minute!
Where did the cow get calcium? Cows, buffalos, elephants, and giraffes get their calcium from the green stuff, and so can we. And, really, calcium is in all plants, especially leafy green vegetables, bok choy, broccoli, cabbage, collard greens, dandelion greens, kale, turnip greens, watercress, and beans! Some plant foods that are highest in calcium include:
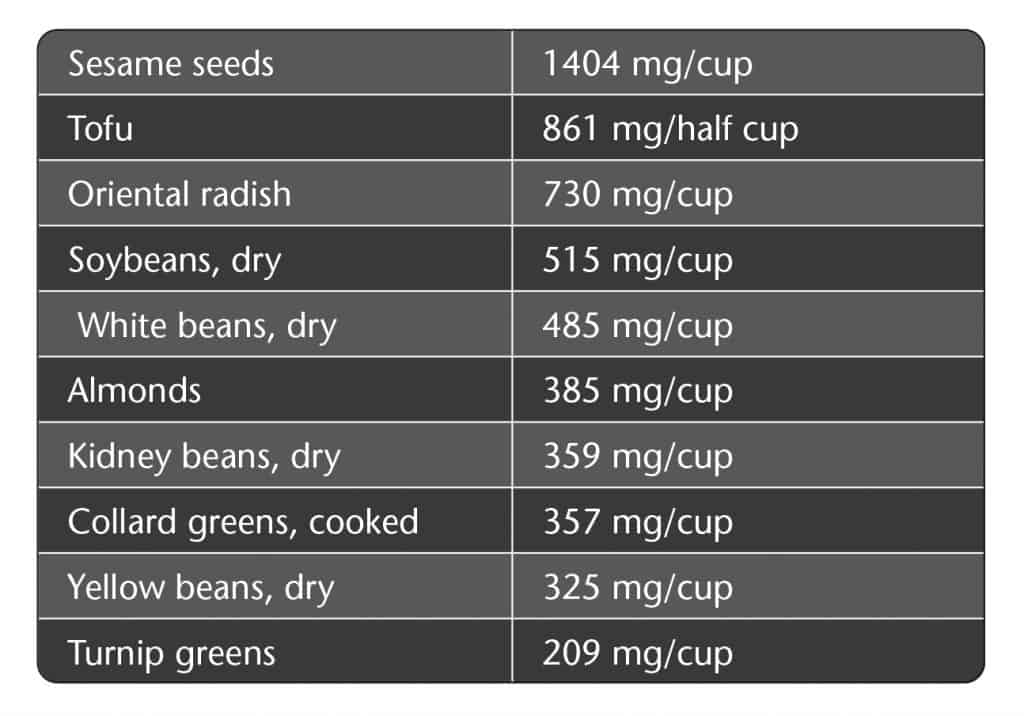
How much calcium do you need every day?
Older people who follow the SAD diet need 1,200 to 1,500 mg per day to maintain calcium balance. But interestingly, those on a 100 percent whole-food, plant-based diet need only 400 to 450 mg per day. (1)

Should you supplement?
People take many different calcium supplements, but these are usually not necessary if you are eating a plant-based diet.
Interestingly, too much calcium may cause trouble. For example, a high intake of calcium has been linked with an increased risk of aggressive prostate cancer, especially in African-American men (2) (from a purely scientific standpoint, this is currently just an association and not a proven cause, but it does give us cause for concern).
You might also be surprised to learn that the association between calcium supplements and fracture prevention is quite weak, and in at least one meta-analysis of studies of older women who took calcium supplements, increased calcium intake showed no clear benefit and even seemed to increase the number of hip fractures. (3)
And, if you’re going to take calcium in pill form, please take magnesium with it. We talk more about magnesium in my book, Eat Plants Feel Whole, but let me just say here that calcium and magnesium are very closely related.
Magnesium supplementation should be around half the amount of the calcium supplement. The two can be purchased in tablets that contain the appropriate mixture. If you get your calcium from plants, magnesium will already be present, and you will not likely have to worry about getting enough.
About the author

Dr. George E. Guthrie is a board-certified family medicine physician and a member of the academic program at AdventHealth’s Centre for Family Medicine in Winter Park, Florida, where he trains medical residents with a focus on community and lifestyle medicine.
Dr. Guthrie became an advocate for lifestyle medicine early in his career while serving on the island of Guam. The high incidence of type 2 diabetes in the population sparked an interest in the effective treatment of chronic disease through lifestyle change.
Dr. Guthrie has helped lead the development of several lifestyle-change programs, including the Complete Health Improvement Project (CHIP), the Wellspring Diabetes Program, and AdventHealth’s CREATION Life program. He is past president of the American College of Lifestyle Medicine. For more information visit DrGeorgeGuthrie.com or EatPlantsFeelWhole.com.
Citations
- R. P. Heaney, J. C. Gallagher et al., “Calcium Nutrition and Bone Health in the Elderly,” American Journal of Clinical Nutrition 36, no. 5 suppl. (Nov. 1982): 986–1013.
- Ken Batai et al., “Race and BMI Modify Associations of Calcium and Vitamin D Intake with Prostate Cancer,” BMC Cancer 17, no. 64 (2017), https://doi.org/10.1186/s12885-017-3060-8.
- Heike A Bischoff-Ferrari, Bess Dawson-Hughes et al. “Calcium Intake and Hip Fracture Risk in Men and Women: A Meta-Analysis of Prospective Cohort Studies and Randomized Controlled Trials,” American Journal of Clinical Nutrition 86 (2007): 1780–90.





Hi there,
I am interested in the statement about plant based eaters needing less calcium than meat eaters. It seems like when the question comes up people say everyone needs the 1200 mg and then say if you just drink fortified milks you should be fine. But what if you don’t drink fortified milks? People throughout history did not drink fortified milks, were they okay or not? I would like to read Dr. Guthries book. I wish my library carried it. Do you know of any other places I could read more about calcium? I’m always wondering if I’m really getting all that my body needs. It’s hard to be “different” from whats “normal”. Thanks for the article.